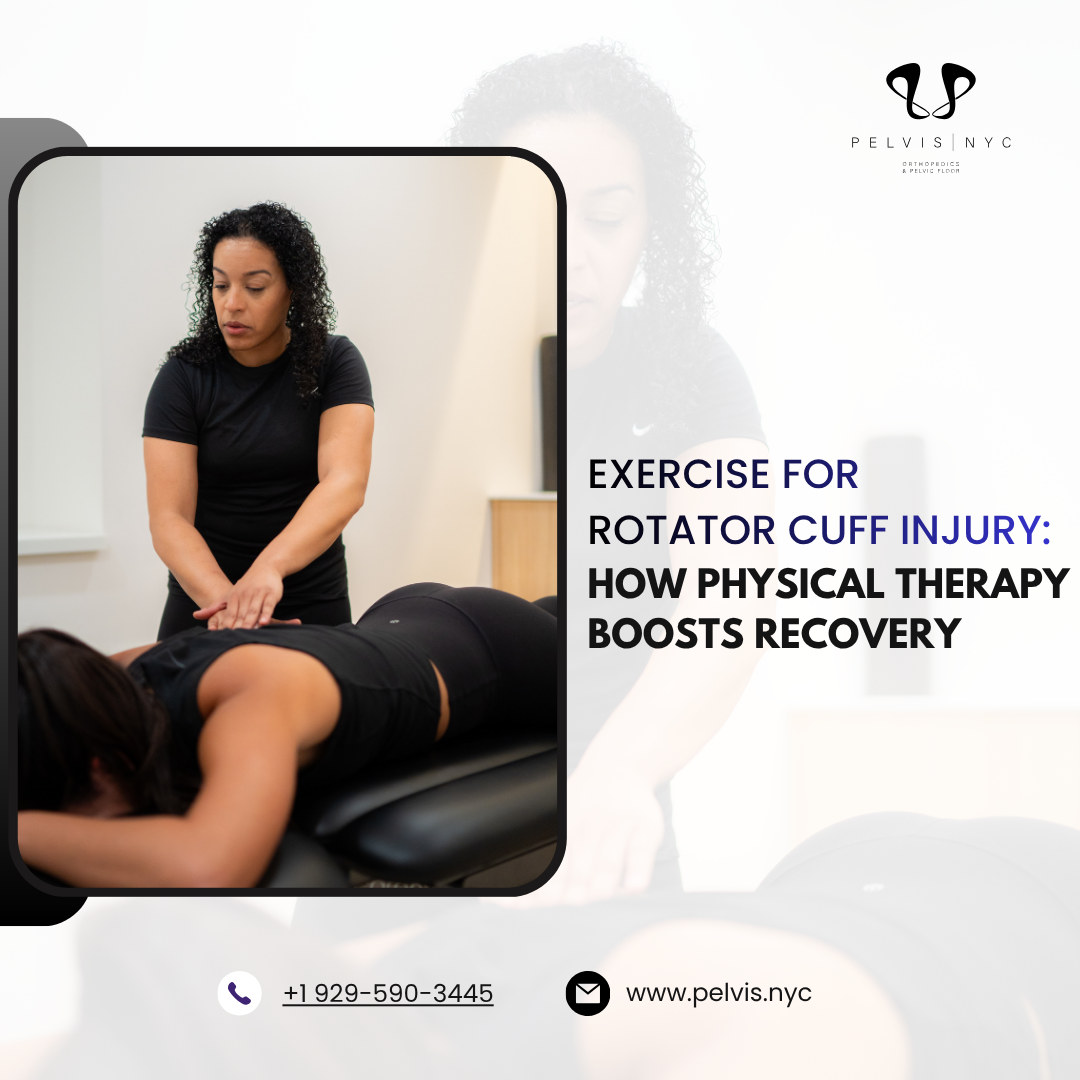
Exercise for Rotator Cuff Injury: What Actually Helps?
Yes—targeted exercise for rotator cuff injury can significantly reduce shoulder pain, improve mobility, and restore strength in both mild and moderate cases. For many people, structured physical therapy helps avoid surgery by improving shoulder stability, muscle coordination, and healing. Before starting any exercise program for a rotator cuff injury, it is essential to consult a doctor for proper assessment and guidance to ensure safe and effective recovery.
The key is choosing the right exercises at the right stage of recovery. Certain movements help strengthen the rotator cuff safely, while others can worsen irritation and delay healing. According to a systematic review, exercise-based rehabilitation is supported by strong evidence as an effective approach for treating rotator cuff injuries.
Most rotator cuff injuries are caused by a combination of overuse and wear and tear over time, particularly in individuals who engage in repetitive overhead activities.
What Is the Rotator Cuff?

The rotator cuff is a group of four muscles and tendons that stabilize the shoulder joint and control arm movement. The rotator cuff connects the shoulder blade (scapula) to the upper arm bone (humerus), which is the main arm bone involved in shoulder movement.
These muscles help with:
- Lifting the arm
- Reaching overhead
- Internal and external rotation
- Shoulder stability during movement
The rotator cuff tendons attach these four muscles to the upper arm bone, allowing for controlled arm movement and stability of the upper arm.
The rotator cuff and shoulder work together constantly during daily activities like:
- Carrying groceries
- Sleeping on your side
- Exercising
- Throwing
- Lifting weights
- Reaching behind your back
Because the shoulder is one of the most mobile joints in the body, it’s also highly vulnerable to injury.
What Causes Rotator Cuff Injuries?
Rotator cuff injuries can happen suddenly or develop gradually over time. Chronic rotator cuff injuries often present as subacromial pain syndrome or shoulder impingement syndrome, which are characterized by shoulder pain during movement. Overuse, repetitive overhead activities, and degeneration can lead to inflammation or tearing of the rotator cuff tendon, while traumatic events like falls or sports injuries may also cause acute damage.
Common Causes Include:
- Repetitive overhead motions
- Heavy lifting
- Weightlifting injuries
- Poor posture
- Aging-related tendon degeneration
- Sports injuries
- Falls or trauma
- Muscle imbalances
- Weak shoulder stabilizers
According to the American Academy of Orthopaedic Surgeons (AAOS), rotator cuff tears become increasingly common with age, especially after 40.
Symptoms of a Rotator Cuff Injury
Symptoms vary depending on severity.
Common Signs Include:
- Shoulder pain when lifting the arm
- Weakness
- Clicking or catching sensations
- Pain at night
- Limited range of motion
- Difficulty reaching overhead
- Pain during exercise
- Shoulder stiffness
A full rotator cuff tear may cause significant weakness and reduced arm function.
Can Exercise Help a Rotator Cuff Injury?

In many cases, yes.
Research shows structured physical therapy is often highly effective for:
- Tendinitis
- Impingement
- Partial tears
- Post-surgical rehabilitation
- Chronic shoulder pain
A study published through the National Institutes of Health (NIH) found that exercise-based rehabilitation significantly improves pain and shoulder function in many patients with rotator cuff disorders.
Why Physical Therapy Is Important for Rotator Cuff Injuries
Many people think resting alone will solve shoulder pain.
Unfortunately, prolonged inactivity often causes:
- Weakness
- Shoulder instability
- Reduced mobility
- Compensatory movement patterns
This is where physical therapy becomes essential.

A licensed physical therapist can identify:
- Muscle imbalances
- Poor shoulder mechanics
- Weak stabilizers
- Mobility restrictions
- Movement compensations
Treatment focuses on restoring normal shoulder function—not just reducing pain. Physical therapy aims to keep the shoulder joint stable by strengthening the rotator cuff and surrounding muscles, which is crucial for preventing further injury. Maintaining a stable shoulder is a key goal of rehabilitation.
Best Exercise for Rotator Cuff Injury Recovery
The best exercises focus on:
- Shoulder stability
- Controlled mobility
- Rotator cuff strengthening
- Scapular control
- Pain-free movement
Below are some of the most commonly recommended exercises in physical therapy.
1. Pendulum Exercise
This is often one of the first exercises used during recovery.
How to Do It
- Lean forward slightly
- Support yourself with one hand
- Let the injured arm hang freely
- Gently swing the arm:
- Forward/backward
- Side to side
- Small circles
Benefits
- Reduces stiffness
- Promotes circulation
- Improves joint mobility
- Minimizes irritation
2. External Rotation with Resistance Band
Shoulder external rotation exercises are critical for strengthening the rotator cuff.
How to do external rotation with a resistance band:
- Attach a resistance band to a stable object at elbow height.
- Stand sideways to the anchor point, holding the band with the hand farthest from the anchor. Keep your elbow bent at 90 degrees and tucked into your side.
- Keeping your elbow close to your body, slowly rotate your forearm outward, away from your torso. Pause, then return to the starting position with control.
- Repeat for 10–15 reps per side.
This shoulder external rotation movement targets the infraspinatus and teres minor, helping to improve shoulder stability and function.
How to Do It
- Attach a resistance band to a stable object
- Keep elbow tucked at your side and keep your elbows straight during the movement to ensure proper form
- Rotate the forearm outward slowly
- Return with control
Benefits
- Strengthens rotator cuff muscles
- Improves shoulder stability
- Reduces injury recurrence
This is one of the most effective exercises for external rotation weakness.
3. Internal Rotation with Resistance Band
Shoulder internal rotation strengthens muscles that stabilize the front of the shoulder.
To perform this exercise, attach a resistance band to a secure anchor at waist height. Stand with your affected arm closest to the anchor, elbow bent at 90 degrees and tucked into your side. Grasp the band and pull it across your body, keeping your elbow close to your waist. Slowly return to the starting position and repeat. Anchoring the band at waist height ensures proper form and safety during the exercise.
Steps
- Stand sideways to the band
- Pull inward toward your stomach
- Keep elbow close to your body
- Move slowly and with control
Why It Helps
- Improves shoulder balance
- Enhances joint control
- Supports healthy movement mechanics
Balancing internal and external rotation strength is essential for recovery.
4. Scapular Retraction Exercise
Many shoulder injuries are actually linked to poor shoulder blade control. One of the best exercises for rotator cuff injury recovery is the shoulder blade squeeze (also known as scapular retraction).
How to do it:
- Sit or stand with your arms at your sides.
- Slowly squeeze your shoulder blades together, pulling them back and down.
- Hold the contraction for a few seconds, then relax.
- Repeat for 10–15 reps.
Benefits: This exercise helps improve posture and shoulder alignment by strengthening the muscles that control the shoulder blades, which is essential for healthy shoulder movement and rotator cuff support.
Instructions
- Sit or stand tall
- Pull shoulder blades gently backward
- Hold for 3–5 seconds
- Repeat slowly
Benefits
- Improves posture
- Supports rotator cuff function
- Reduces shoulder strain
5. Wall Slides
Excellent for improving shoulder mobility without excessive strain. Wall push-ups are a great exercise for beginners or those recovering from pain, as they help build shoulder stability without putting too much stress on the joint. For those with limited strength, using a sturdy chair for support can make wall push-ups even easier. In addition to targeting the shoulders, wall push-ups also engage the chest muscles, helping to build upper body strength.
How to Perform
- Stand facing a wall
- Place forearms on the wall
- Slowly slide arms upward
- Avoid shrugging shoulders
Benefits
- Improves overhead mobility
- Activates stabilizing muscles
- Encourages proper movement patterns
6. Isometric Shoulder Exercises
These are especially useful during early-stage recovery. For example, isometric shoulder extension is a valuable exercise at this stage, as it allows you to engage the shoulder muscles without moving the joint, helping to build strength safely.
Example: Isometric External Rotation
- Press your hand gently against a wall
- Engage muscles without moving the arm
- Hold for 5–10 seconds
Why It Works
- Builds strength safely
- Minimizes tendon irritation
- Helps reduce pain
What Exercises Should You Avoid?
Not every shoulder exercise is safe during recovery.
Avoid:
- Heavy overhead pressing
- Behind-the-neck exercises
- Aggressive stretching
- High-volume throwing
- Heavy lifting
- Painful movements
- Deep dips
Pain during exercise is often a sign that the tissue is not ready yet.
How Long Does Recovery Take?
Recovery depends on:
- Severity of injury
- Age
- Activity level
- Consistency with rehab
- Whether surgery was required
Average Recovery Timeline
| Condition | Recovery Time |
| Mild strain | 2–6 weeks |
| Tendinitis | 6–12 weeks |
| Partial tear | 2–4 months |
| Post-surgical rehab | 4–9 months |
Consistency matters more than intensity.
When Does a Rotator Cuff Tear Require Surgery?
Not all tears require surgery.
Many partial tears improve with:
- Physical therapy
- Strengthening exercises
- Activity modification
- Manual therapy
However, some injuries may require surgery if there is:
- Complete tendon rupture
- Significant weakness
- Persistent pain
- Failed conservative treatment
- Loss of function
What Is Arthroscopic Rotator Cuff Repair?
Arthroscopic rotator cuff repair is a minimally invasive surgical procedure used to repair torn tendons.
During surgery:
- Small incisions are made
- A camera guides the procedure
- Damaged tendons are repaired with anchors
Compared to traditional open surgery, arthroscopic procedures often lead to:
- Smaller scars
- Less tissue damage
- Faster early recovery
But surgery alone is not enough.
Why Physical Therapy After Surgery Is Essential

After arthroscopic rotator cuff repair, physical therapy is critical for:
- Restoring mobility
- Preventing stiffness
- Rebuilding strength
- Protecting the repair
- Regaining shoulder function
Post-surgical rehab typically progresses through phases:
Phase 1: Protection
- Sling use
- Gentle passive motion
Phase 2: Mobility
- Assisted movement
- Light stretching
Phase 3: Strengthening
- Resistance exercises
- Rotator cuff activation
Phase 4: Return to Activity
- Functional training
- Sport-specific movement
Skipping rehab significantly increases reinjury risk.
The Connection Between Posture and Rotator Cuff Pain
Many rotator cuff problems are worsened by posture.
Poor posture can:
- Narrow shoulder space
- Increase tendon irritation
- Reduce shoulder stability
Common contributors include:
- Desk work
- Rounded shoulders
- Forward head posture
- Weak upper back muscles
Physical therapy often addresses these underlying movement issues—not just shoulder pain itself.
Can You Exercise with a Rotator Cuff Injury?
Usually yes—but carefully.
The goal is not complete rest.
Instead:
- Avoid aggravating movements
- Stay active within tolerance
- Focus on controlled rehabilitation
A structured rehab plan is safer and more effective than random online exercises.
Real Recovery: Why Guided Rehab Works Better
One of the biggest mistakes people make is trying to “push through” shoulder pain.
Successful recovery requires:
- Proper diagnosis
- Progressive strengthening
- Mobility restoration
- Movement retraining
- Patience
This is why working with a skilled physical therapist matters.
Why Pelvis NYC Can Help

At Pelvis NYC, physical therapists take a whole-body approach to recovery and movement rehabilitation.
Their team helps patients:
- Recover from shoulder injuries
- Improve mobility
- Restore strength
- Reduce chronic pain
- Return to exercise safely
Whether you’re recovering from a rotator cuff strain, chronic shoulder pain, or post-surgical rehab, personalized physical therapy can help speed recovery and prevent future injury.
👉 Early treatment often leads to better long-term outcomes.
Final Thoughts
The best exercise for rotator cuff injury recovery is one that restores strength, mobility, and shoulder stability without increasing pain.
In many cases, physical therapy can help patients avoid surgery entirely—or recover more successfully after surgical repair.
If shoulder pain is limiting your workouts, sleep, or daily activities, don’t ignore it. Addressing the problem early can prevent chronic dysfunction and long-term weakness.
Frequently Asked Questions (FAQs)
What is the best exercise for a rotator cuff injury?
External rotation exercises with a resistance band are among the most effective for strengthening the rotator cuff safely. For optimal muscle activation and safety, keep your arm at shoulder height while performing these exercises.
Can exercise heal a rotator cuff tear?
Partial tears often improve with physical therapy and strengthening exercises. Complete tears may require surgery.
Should I stretch a rotator cuff injury?
Gentle mobility exercises can help, but aggressive stretching may worsen symptoms.
How long does rotator cuff recovery take?
Mild injuries may improve in weeks, while surgical recovery can take several months.
Can physical therapy prevent shoulder surgery?
Yes. Many patients improve significantly with structured rehabilitation and never require surgery.
What causes rotator cuff injuries?
Common causes include overuse, repetitive overhead activity, repetitive shoulder rotation (especially during sports or work activities), poor posture, aging, and sports injuries.