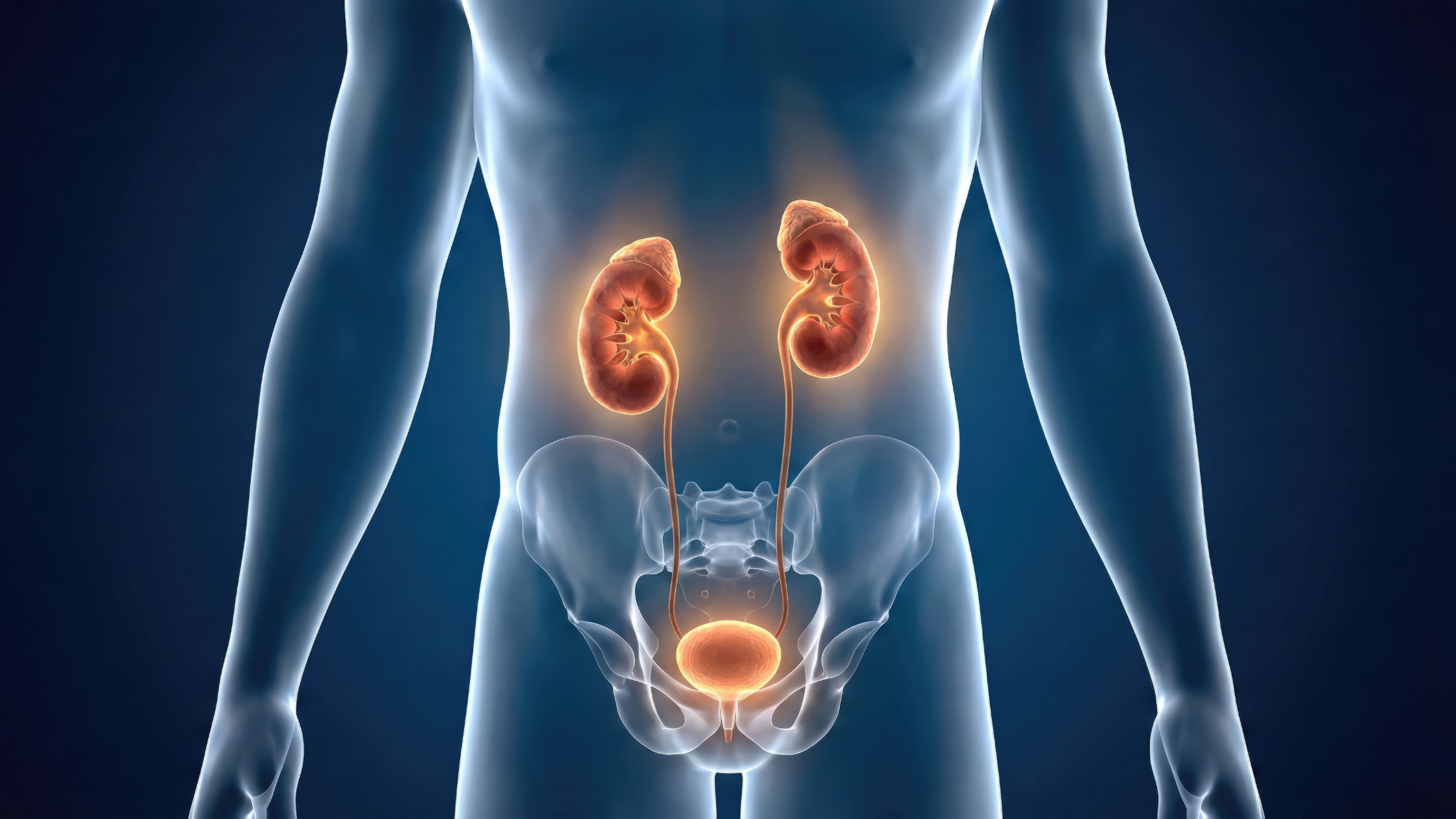
What Causes Urinary Incontinence in Males — and Can It Be Treated?
Urinary incontinence in males is the involuntary leakage of urine, often caused by pelvic floor weakness, prostate surgery, nerve dysfunction, or bladder overactivity. Urinary incontinence can be short-term or long-lasting (chronic). The good news is that most men — especially between ages 21–48 — improve significantly with conservative treatment like pelvic floor physical therapy and bladder retraining before surgery is ever considered.
If you’re leaking urine, avoiding workouts, or constantly mapping out bathrooms, you’re not alone — and this is fixable. If urinary incontinence is frequent or affects your daily activities or quality of life, it’s important to seek medical advice. Understanding risk factors for developing urinary incontinence, such as bladder outlet obstruction, neurological disease, and cognitive impairment, is important for preventing or addressing this condition.
What Is Urinary Incontinence in Males?
Urinary incontinence refers to accidental urine leakage. While more common in older men, studies show that up to 11% of men under 50 experience some form of bladder control issue, according to research published in Urology.
In men aged 21–48, incontinence often relates to:
- Pelvic floor muscle dysfunction
- Prostate procedures
- Athletic strain or heavy lifting
- Chronic stress and muscle tension
- Overactive bladder patterns
In older men, the most common cause of urinary incontinence is benign prostatic hyperplasia (BPH), which occurs when the prostate grows and squeezes the urethra. This bladder outlet obstruction can contribute to symptoms like detrusor overactivity and post-prostatectomy incontinence.
It’s common — but it’s not something you just have to “live with.”
Symptoms and Diagnosis of Male Urinary Incontinence
Recognizing the symptoms of urinary incontinence in men is the first step toward effective treatment and management. Common signs include leaking urine during activities that put pressure on the bladder, such as coughing, sneezing, or lifting heavy objects. Some men may also notice a sudden, intense urge to urinate that is difficult to control, leading to accidental leakage. These symptoms can vary depending on the type of urinary incontinence—whether it’s stress urinary incontinence, urge incontinence, or mixed incontinence.
Diagnosing male urinary incontinence requires a thorough evaluation by a healthcare provider. This process typically begins with a detailed medical history and a physical exam to identify potential contributing factors. Your provider may ask about your urinary habits, fluid intake, and any previous surgeries or medical conditions. Diagnostic tests, such as urodynamic studies or cystoscopy, may be recommended to assess bladder function and rule out other urinary tract issues.
A precise diagnosis is essential because each type of urinary incontinence in men—whether stress, urge, or mixed—requires a unique management strategy. By working closely with your healthcare provider and undergoing a comprehensive evaluation, you can identify the underlying cause of your symptoms and develop a targeted treatment plan to regain bladder control and improve your quality of life.
Types of Urinary Incontinence in Men
Understanding your type of leakage helps determine the best treatment. Some men may experience chronic urinary incontinence, which is a long-lasting condition that may require ongoing management.
1. Stress Incontinence in Men
Stress incontinence occurs when physical pressure overwhelms the urinary sphincter or pelvic floor muscles.
It often happens during:
- Coughing
- Sneezing
- Heavy lifting
- Running or jumping
- Core exercises
In men, stress incontinence commonly develops after prostate surgery due to changes at the bladder neck and surrounding support structures. Prostate removal can damage the sphincter muscle, which controls the flow of urine, leading to bladder leakage. The majority of male urinary incontinence cases are secondary to sphincter weakness following prostatic surgery.
Why It Happens
The bladder neck and urethral sphincter act as a valve system. Nerve signals regulate the function of the urinary bladder and sphincter muscles, coordinating urination and continence by ensuring the muscles contract and relax at the right times. If that valve weakens — or if the pelvic floor muscles cannot support it — leakage occurs under pressure.
2. Overactive Bladder & Urge Incontinence
Overactive bladder (OAB) is characterized by sudden urgency, frequency, and sometimes urge incontinence.
This is less about muscle weakness and more about:
- Bladder muscle overactivity
- Nervous system hypersensitivity
- Poor coordination between bladder and pelvic floor
Treatment focuses heavily on:
- Bladder training
- Nervous system regulation
- Coordinated pelvic floor control
3. Overflow Incontinence
Overflow incontinence occurs when the bladder does not empty completely, leading to dribbling or constant leakage.
Common causes include:
- Prostate enlargement
- Nerve dysfunction
- Bladder outlet obstruction
- Weak bladder contraction
- Bladder dysfunction
Men with overflow symptoms often report:
- Weak urine stream
- Hesitancy
- Feeling of incomplete emptying
- Urinary retention
Detrusor overactivity occurs in about 75% of men with benign prostatic hyperplasia.
This type requires medical evaluation to rule out obstruction before starting pelvic floor therapy.
4. Mixed Incontinence
Mixed urinary incontinence combines features of both stress and urge incontinence, meaning a person may experience leaking when lifting weights as well as sudden uncontrollable urges.
Pelvic floor therapy is the most widely recommended non-invasive treatment for male urinary incontinence, including mixed urinary incontinence. Treatment requires addressing both muscle support and bladder signaling.
5. Functional Incontinence
Functional incontinence is less about bladder or pelvic floor dysfunction and more about access barriers.
It can occur when:
- Mobility issues prevent reaching the bathroom in time
- Orthopedic injuries slow movement
- Environmental obstacles interfere
- Neurological disease impairs the ability to reach the bathroom in time, increasing the risk of functional incontinence
In younger men (21–48), this is less common but may occur after injury or surgery.
How the Bladder Neck & Pelvic Floor Work Together
The bladder neck acts as an internal valve. The pelvic floor muscles support and reinforce that valve externally.
When functioning properly:
- The bladder fills
- The bladder neck remains closed
- The pelvic floor provides support
- Urination occurs voluntarily
Bladder storage capacity and control are crucial for maintaining continence, as they ensure the bladder can hold urine until voluntary voiding occurs.
When coordination breaks down, male urinary incontinence can develop. Voiding dysfunction can disrupt the coordination between the bladder and pelvic floor, leading to incontinence.
This is why pelvic floor therapy is often central to recovery.
Treatment for Urinary Incontinence in Males
Treatment is tailored to the incontinence type, severity, and underlying cause. Most men benefit from conservative, non-surgical approaches first.

1. Pelvic Floor Physical Therapy
- Strengthens muscles supporting the bladder and urethra
- Improves sphincter timing and coordination
- Reduces urgency and leakage
- Supervised training improves outcomes
2. Bladder Retraining
- Gradually increases bladder capacity
- Reduces urgency frequency
- Restores nervous system coordination
3. Lifestyle Adjustments
- Limit caffeine, alcohol, and bladder irritants
- Maintain hydration without overloading the bladder
- Support bowel regularity and healthy weight
4. Incontinence Pads
- Provide temporary support during recovery
- Do not address underlying dysfunction
5. Medications
- Anticholinergics for urge symptoms
- Alpha-blockers if enlarged prostate contributes to obstruction
6. Surgical Options
Reserved for men who do not respond to conservative therapy:
- Artificial Urinary Sphincter: Gold standard for severe post-prostatectomy stress incontinence
- Male Sling Surgery: Supports urethra to reduce leakage during physical activity
Managing Mixed Incontinence in Men
For mixed incontinence, a combination approach is most effective:
- Bladder training for urgency control
- Pelvic floor exercises for stress support
- Lifestyle modifications to reduce bladder irritation
- Medications if necessary
- Surgery only if conservative therapy fails
With a personalized treatment plan, most men achieve significant improvement and regain confidence.
Why Choose Pelvis NYC for Urinary Incontinence in Males?

At Pelvis NYC, we specialize in pelvic floor physical therapy for men.
Our approach includes:
- Comprehensive evaluation
- Evidence-based pelvic floor muscle training
- Bladder retraining programs
- Strength and coordination retraining
- Respectful, private, patient-centered care
We understand the stigma men face around bladder control problems — and we approach care with professionalism and discretion.
👉 Schedule a consultation with Pelvis NYC to start a personalized treatment plan designed for your body and goals.
Most men improve without surgery. Early treatment makes the biggest difference.
Frequently Asked Questions
What causes urinary incontinence in males?
Common causes include pelvic floor weakness, prostate surgery, nerve dysfunction, and overactive bladder.
Can pelvic floor therapy fix male incontinence?
Yes. Many men see significant improvement or full resolution with supervised therapy.
Is urinary incontinence normal in younger men?
It’s not uncommon, but it’s not normal — and it’s treatable.
How long does pelvic floor therapy take?
Most men see improvements within 4–8 weeks, depending on severity.
When is surgery necessary?
Surgery is typically considered only after conservative treatments fail.
Key Takeaway on Male Urinary Incontinence Types
Urinary incontinence in males is highly treatable — but only when the type is properly identified.
- Stress incontinence → Support & strength
- Overactive bladder → Nervous system & bladder retraining
- Overflow incontinence → Evaluate obstruction first
- Mixed incontinence → Combination therapy
- Functional incontinence → Address mobility barriers
Pelvic floor dysfunction is often part of the picture — which is why conservative therapy remains the foundation of treatment.
Related Blog: Therapy for Urinary Incontinence: Know How Pelvic Floor Therapy Works