A Physical Therapist’s Take on BPH Treatment, Sexual Function & Recovery
Can UroLift Cause Erectile Dysfunction?
Let’s tackle this right out of the gate—can Urolift cause erectile dysfunction?- the short answer is no. The UroLift System is designed to relieve urinary symptoms caused by BPH (Benign Prostatic Hyperplasia) without affecting erectile function. Clinical studies show that UroLift does not cause new, sustained erectile dysfunction, setting it apart from other BPH treatments.
As a pelvic health PT, I work with men post-procedure and see firsthand that erectile dysfunction (ED) after UroLift is rare and typically unrelated to the procedure itself.
But does that mean it never affects your performance? Not exactly.
While the mechanical side of erections remains safe, some men report temporary issues due to:
- Pelvic floor tension
- Anxiety
- Post-op inflammation
- Pre-existing sexual health concerns
Most of this is manageable with pelvic rehab, relaxation techniques, and time. Importantly, UroLift is not associated with new sexual dysfunction, and the treatment effect on sexual function is minimal compared to other BPH therapies like TURP or laser, which have higher rates of sexual side effects.
What You Should Know About Erectile Dysfunction
ED is complex—it’s not just about the penis; it’s about nerves, blood flow, pelvic floor muscles, emotions, and overall health.
From my clinical perspective, men who experience ED post-UroLift often:
- Already had mild ED
- Are dealing with stress, performance anxiety, or prostate-related tension
- Experience tight pelvic muscles that interfere with function
The good news? Physical therapy can help. We work on improving blood flow, relaxing the pelvic floor, and restoring confidence.
Understanding BPH Treatment and Sexual Health
BPH affects about 50% of men over age 50, and the number one symptom is disrupted urination—urgency, frequency, dribbling, or incomplete emptying.
Unfortunately, many treatments for BPH have a dark side: they can mess with your sex life.
Common BPH treatments and their sexual side effects:
| Treatment | Invasive? | Risk of ED? | Risk of Retrograde Ejaculation? |
| TURP | Yes | Moderate | High |
| Laser therapy | Yes | Moderate | Moderate |
| Medications (alpha-blockers, 5-ARIs) | No | Possible | Low–Moderate |
| UroLift | No | Very Low | Very Low ✅ |
Therapies such as TURP, laser, and even medication are associated with a higher risk of sexual side effects, including erectile and ejaculatory dysfunction, compared to UroLift®. UroLift® stands out as a minimally invasive alternative to traditional surgical options, with clinical data showing it does not cause new or lasting ejaculatory dysfunction.
Why Sexual Function Matters in BPH Treatment
It’s not just about urination—it’s about feeling like yourself again.
As a therapist, I’ve seen men recover their urinary confidence but still feel “off” because of unexpected sexual challenges. That’s why sexual function should always be part of the conversation around BPH treatment options.
UroLift shines here because it:
- Preserves erectile function
- Maintains ejaculation
- Doesn’t involve hormones or cutting tissue
- Allows for quicker recovery compared to invasive procedures
- Helps patients avoid major surgery and is a safer alternative to most traditional surgical options
Exploring BPH Treatment Options (The Balanced View)
Before committing to a treatment, it’s wise to understand your options. It’s important to consider other BPH treatment options, such as medications, minimally invasive procedures, and traditional surgeries, to find what best fits your needs.
Medications
Medications are often the first line of therapy for BPH. BPH medications, such as alpha-blockers and 5-alpha-reductase inhibitors, can help relieve symptoms by relaxing the muscles of the prostate and bladder or by shrinking the prostate. However, some patients may experience side effects or may not achieve sufficient relief with medication alone.
Ultimately, the best approach is chosen after you and your doctor decide together based on your symptoms and preferences.
✅ Lifestyle + Watchful Waiting
Mild symptoms? Start here. Diet, hydration, bladder training, and pelvic floor therapy can help.
✅ Medications
Options like tamsulosin or finasteride, which are examples of BPH medications, are common but can cause dizziness, low libido, or ED in some men.
✅ Surgical Interventions
- TURP: Effective but carries sexual side effects
- Laser therapy: Less invasive than TURP but still risky
- Prostatic urethral lift (UroLift): A minimally invasive treatment performed as an outpatient procedure, office-based, and sex-sparing
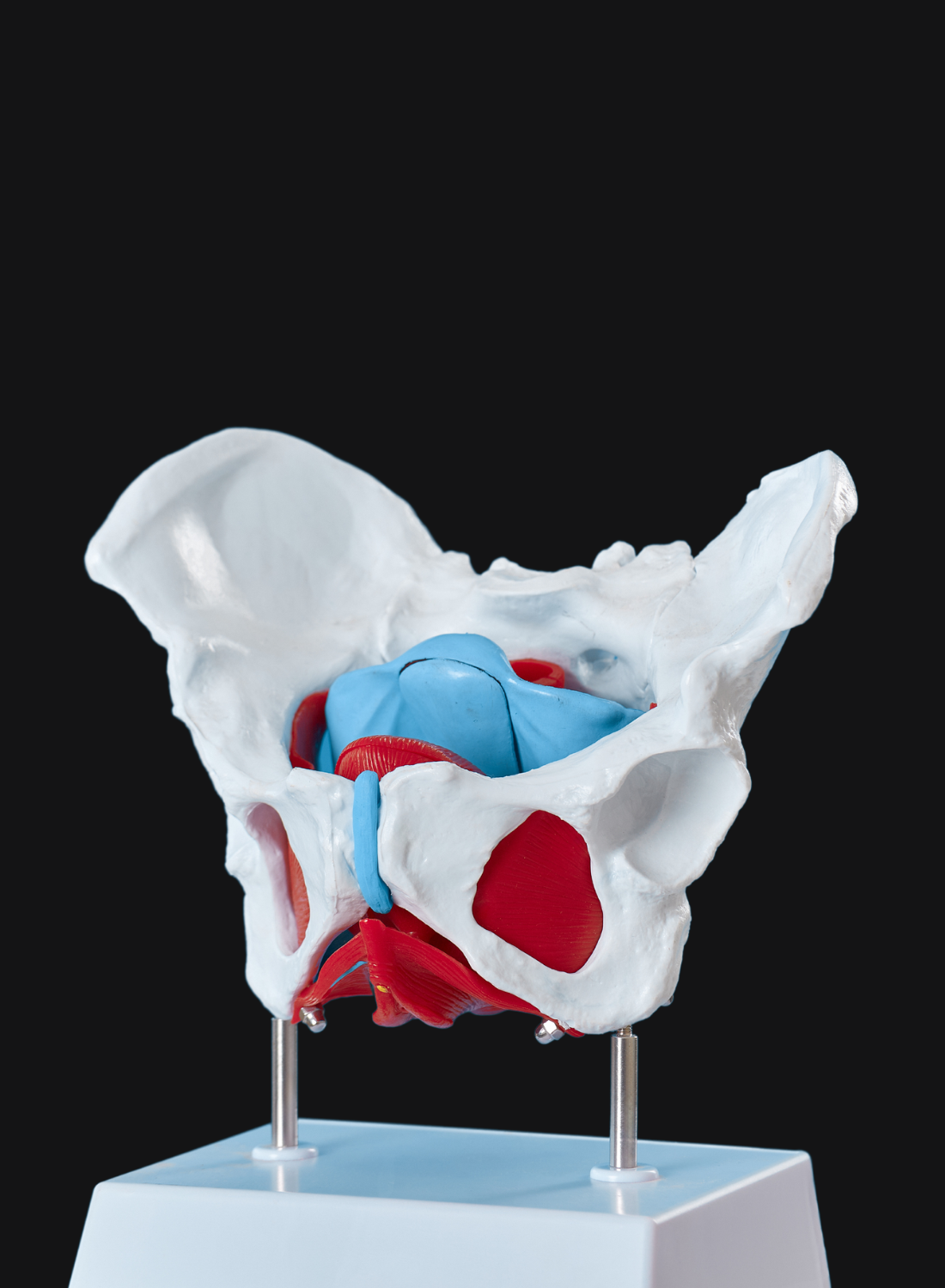
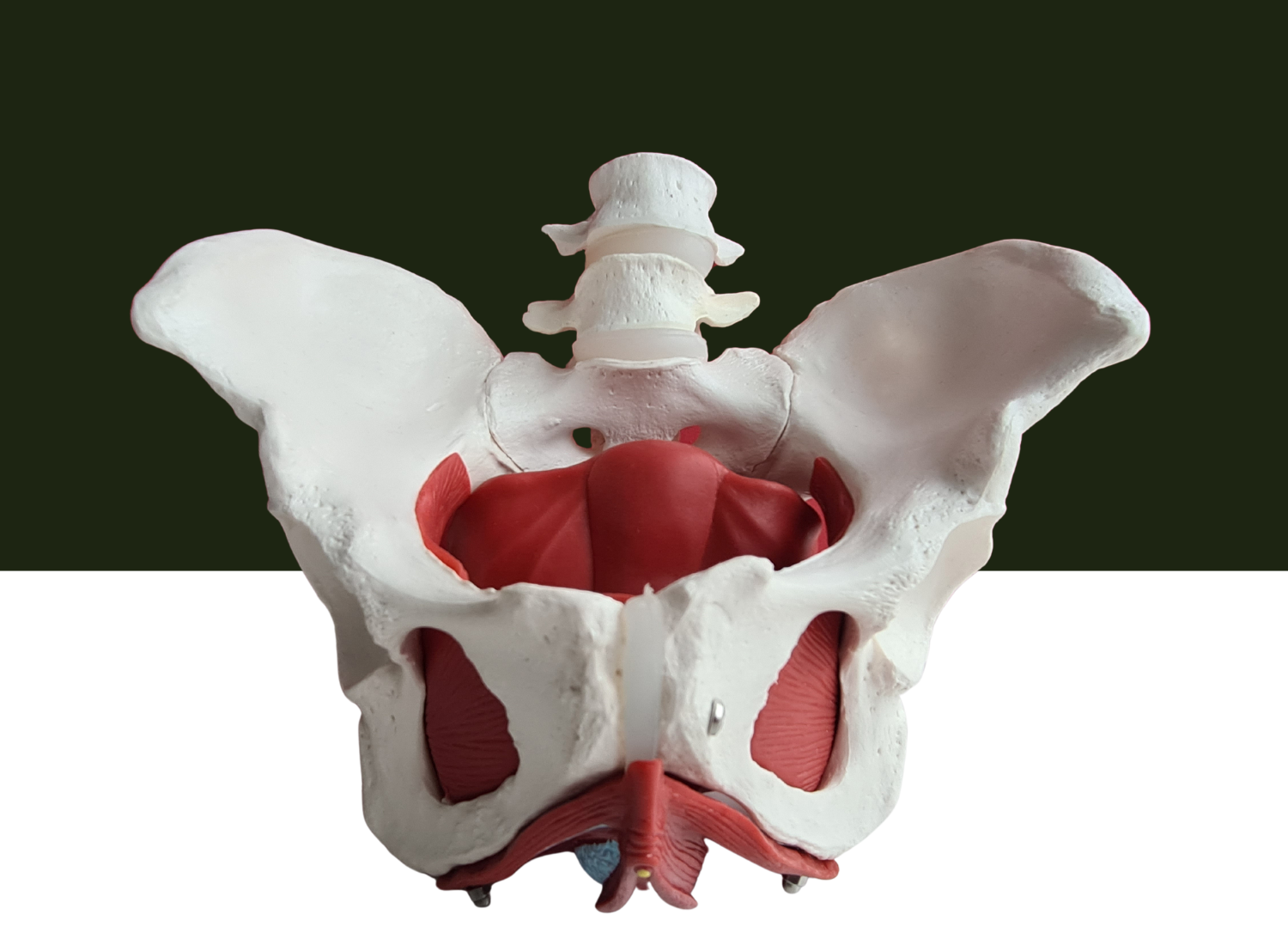
What Is the Prostatic Urethral Lift (UroLift System)?
The UroLift System deploys permanent implants made from standard surgical implantable materials to lift and hold prostate tissue away from the urethra. Think of it like opening curtains to let urine flow freely again.
Why Patients Love It:
Patients typically experience a quick recovery, minimal side effects, and preservation of sexual function after UroLift, making it a preferred choice for many.
- No hospital stay
- No cutting
- No catheter (in most cases)
- Sexual function stays intact
- Quick return to work and life
For men who are sexually active and concerned about side effects, UroLift is often the first-line option I recommend in collaboration with their urologist.
Minimally Invasive with Solid Clinical Data
UroLift is FDA-approved and backed by some of the most robust clinical data in the BPH space. Clinical studies have demonstrated the effectiveness of UroLift as a minimally invasive treatment for treating BPH, providing evidence-based support for its safety and efficacy.
Key Stats from Clinical Trials:
- 5-year data shows durable symptom relief
- Patients report symptom relief after UroLift treatment
- No new cases of ED reported in trials
- High patient satisfaction
- Improved urinary flow and quality of life
If you’re into data (and who isn’t when it’s your body), here’s what one of the leading studies showed:
“Erectile and ejaculatory function were preserved in 100% of sexually active men treated with UroLift.” — Journal of Sexual Medicine, 2019
How This Treatment Affects Daily Life
The goal of any BPH procedure shouldn’t just be symptom relief—it should be a return to normal life, including:
- Better sleep (less nighttime peeing)
- More confidence in social settings
- Renewed sexual energy
- Less anxiety about “accidents”
After UroLift, the most common side effects include urinary discomfort, pelvic pain, burning with urination, and blood in the urine. Most symptoms are mild to moderate and typically resolve within a few weeks. Symptoms related to the procedure are temporary, and most patients have their symptoms resolved within a short period.
Most of my patients report feeling lighter, more in control, and more themselves within weeks of UroLift.
And when they pair it with pelvic physical therapy? The results are even better.
What to Expect During UroLift Treatment
If you’re considering the UroLift System, you’ll be glad to know it’s a minimally invasive procedure designed with your comfort and convenience in mind. The entire treatment usually takes less than an hour, and it’s performed right in your urologist’s office or an ambulatory surgery center.
Here’s how it works: Using the UroLift delivery device, your doctor will deploy tiny, permanent implants that gently lift and hold the enlarged prostate tissue away from your urethra. This relieves the obstruction caused by benign prostatic hyperplasia (BPH) and allows urine to flow more freely—no cutting or removal of prostate tissue required.
The procedure can be done under local or general anesthesia, depending on your needs and your doctor’s recommendation. Most patients experience only minimal discomfort, and you’ll typically be able to go home the same day—often without the need for a catheter. Many patients experience symptom relief within just a few weeks after the procedure, and you can expect to get back to your normal routine quickly.
For men looking for a straightforward, effective way to address BPH symptoms and enlarged prostate tissue, UroLift offers a path to symptom relief with minimal downtime and a fast return to daily life.
Finding the Right Healthcare Provider for UroLift
Selecting the right healthcare provider is a crucial step in your journey to relief from BPH symptoms. The UroLift System consists of a specialized delivery device and permanent implants, and it’s important to choose a urologist who is experienced in performing this minimally invasive procedure.
Start by asking your primary care physician for a referral or searching online for urologists in your area who offer the UroLift System treatment. Look for providers who have a track record of success with the procedure and who can clearly explain how the UroLift System works to relieve obstruction caused by enlarged prostate tissue.
A knowledgeable provider will answer all your questions about benign prostatic hyperplasia, the UroLift System, and what to expect before, during, and after treatment. By partnering with an experienced urologist, you’ll be setting yourself up for the best possible outcome—achieving symptom relief and getting back to your life with confidence.
The Role and Importance of Physical Therapy in the Question: Can Urolift Cause Erectile Dysfunction?
As a pelvic health physical therapist, I’ve seen how targeted rehab can make a huge difference post-UroLift.
PT addresses pelvic floor tension, improves circulation, reduces anxiety, and promotes healthy muscle coordination. We also help men regain confidence and sexual function after BPH treatments. Personalized therapy programs can accelerate recovery, reduce post-operative discomfort, and improve outcomes for both urinary and sexual health.

Rehab with Pelvic Floor Therapy After UroLift
Recovery doesn’t end once the UroLift procedure is over — rehab is where your body integrates the change. That’s why pelvic floor therapy is so valuable in the post-op phase.
I work with men to retrain muscles that may have been compensating for years of straining or dysfunction. After UroLift, some patients develop tightness, guarding, or overactive muscles as their body adjusts to the improved urinary flow. Addressing this early leads to better long-term outcomes.
What does rehab look like?
Typical post-UroLift pelvic floor rehab may include:
- Pelvic floor relaxation and retraining exercises
- Manual therapy for the lower back, hips, and perineum
- Breathwork and core coordination drills
- Education on bladder habits, voiding posture, and fluid timing
Many men are surprised by how much PT can enhance their confidence—not just physically, but sexually and emotionally too. Think of it as the final step in reclaiming your comfort, control, and quality of life after BPH treatment.
Final Thoughts on Can Urolift Cause Erectile Dysfunction
If you’re on the fence about UroLift, here’s my take:
If you want to fix your flow and keep your mojo, it’s one of the best options out there.
But don’t go it alone.
Discomfort varies greatly between individuals, but the procedure typically helps minimize discomfort for most patients.
Talk to your urologist. Talk to a pelvic therapist. Support your recovery, mentally and physically, and you’ll be back to peak performance in no time.Ready to take the next step? Visit Pelvis NYC to schedule a consultation with a specialist who understands your body and your goals.