Let’s talk about sexual health – a complex and multifaceted aspect of overall wellness, influenced by personal, psychological, relational, cultural, spiritual, physical, and emotional factors. According to official sources, such as the World Health Organization, the definition of it is a state of physical, emotional, mental, and social well-being in relation to sexuality, not merely the absence of disease or dysfunction.
To define it, it is as individual and complicated as the various dynamics of our lives, encompassing the ability to have pleasurable and safe sexual experiences, free of coercion, discrimination, and violence, and involves a positive and respectful approach to sexual relationships. Sexual rights are fundamental to achieving sexual health, ensuring that everyone can experience sexuality free from discrimination and violence.
What is Sexual Health?
Clear definitions of sexual health, sexuality, and sexual rights are essential for understanding this topic. These definitions help clarify that it is shaped by societal, legal, and community factors and is not limited to individual experiences.
To define it, it is as individual and complicated as the various dynamics of our lives, encompassing the ability to have pleasurable and safe sexual experiences, free of coercion, discrimination, and violence, and involves a positive and respectful approach to sexual relationships. Importantly, sexual health is not just the absence of disease or dysfunction, but a holistic state of well-being.
Recognizing the diversity of human sexuality is crucial, as it underscores the importance of sexual health as an important part of overall wellness. It requires a positive, respectful, and rights-based approach to sexuality, including the possibility of having pleasurable and safe sexual experiences, free from coercion and discrimination.
Sexual health is interconnected with both emotional health and mental health, highlighting the importance of a holistic approach to well-being. Intimacy and relationship dynamics also play a significant role in sexual health, whether one is single, dating, or in a committed relationship.
As a physical therapist, I’ve seen firsthand patients struggling with sexual dysfunction– whether it’s pain during intercourse, difficulty achieving orgasm, or urinary incontinence during sex.
Many of these patients are surprised to learn that the root cause of their problems may be their pelvic floor muscles. But the good news is that with the right care and exercises, you can improve the health of your pelvic floor muscles and enhance your sexual well-being. So let’s explore the connection between sexual health and pelvic floor muscles!
Introduction to Pelvic Floor Muscles
Pelvic floor muscles are fundamental to both sexual health and overall well-being. Often referred to as the pubococcygeus muscles, these muscles form a supportive hammock for the pelvic organs, playing a vital role in controlling urinary and bowel functions. A strong pelvic floor not only helps prevent sexual dysfunction but also enhances sexual pleasure by improving sensation and response during sexual activity. Maintaining pelvic floor health is especially important during the reproductive years, as it supports overall health, social well-being, and mental health. Regular exercises, such as Kegels, can strengthen these muscles, contributing to improved physical and mental health, and helping individuals enjoy a more satisfying and pleasurable sex life. Prioritizing pelvic floor health is a key step toward achieving optimal well-being and reducing the risk of sexually transmitted infections.
Anatomy of the Pelvic Floor Muscles and Reproductive Health
To understand why pelvic floor muscles are important for sexual health, it’s essential to know their anatomy. The pelvic floor is a group of muscles that stretch from the pubic bone at the front of the pelvis to the tailbone at the back. These muscles form a sling that supports the bladder, rectum, and other pelvic organs.
Sexual health risks, such as sexually transmitted infections (STIs) and unplanned pregnancies, can vary significantly by age. Young adults, especially those by the age of 25, often face higher rates of STIs and unplanned pregnancies compared to other age groups.
Sexual orientation can influence sexual health, making it important to understand and respect different orientations. This includes recognizing how someone is attracted sexually, emotionally, and romantically, and acknowledging that sexual orientation can be fluid and change over time.
Access to contraception is a crucial part of comprehensive reproductive health services, helping individuals make informed choices about family planning and reducing barriers to sexual health care.
How Pelvic Floor Muscles Affect Sexual Health and Sexual Relationships
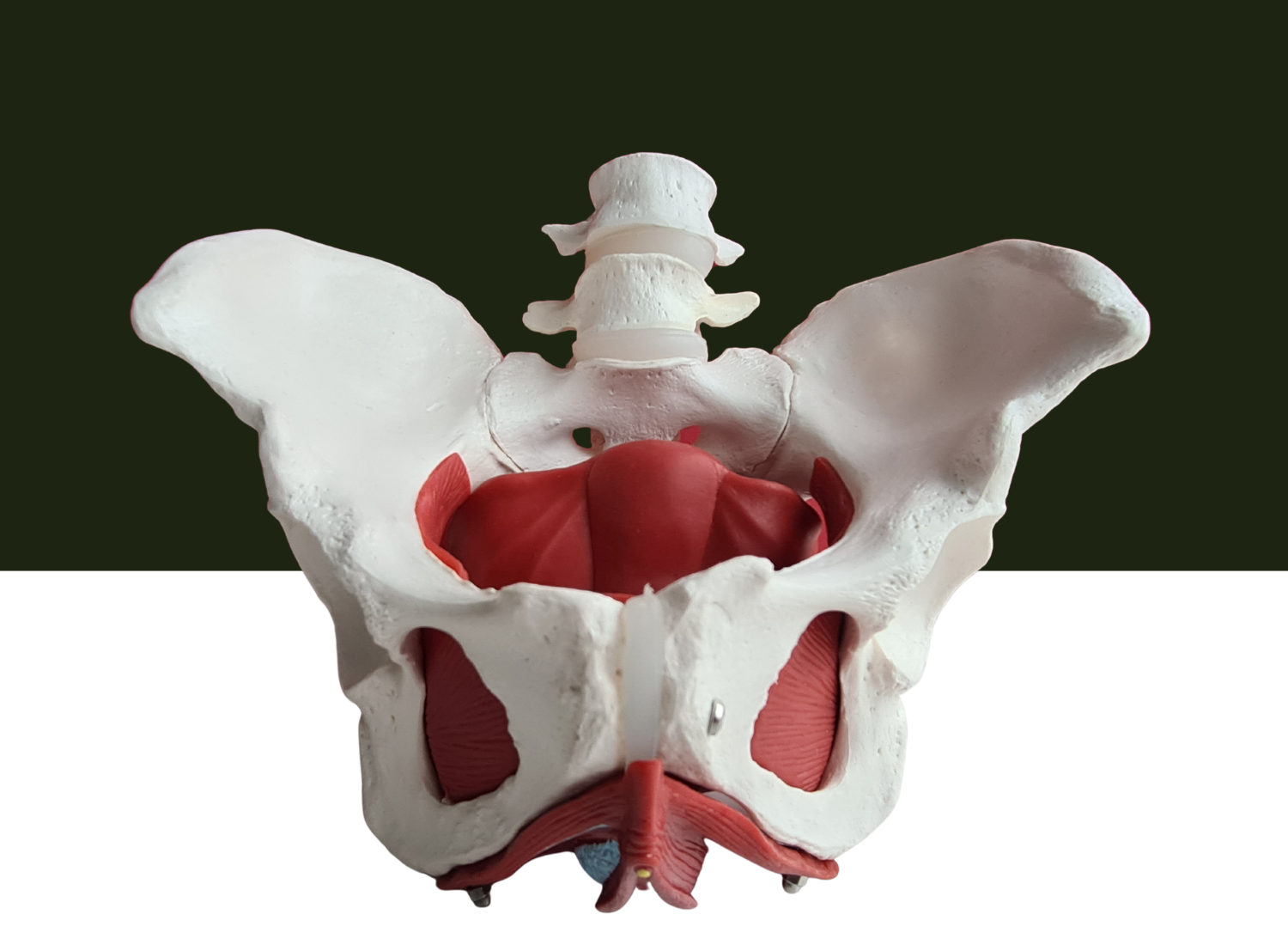
So why do pelvic floor muscles matter for sexual health? The answer lies in their role in sexual function. The pelvic floor muscles play a crucial role in achieving and maintaining an erection in men. Strong pelvic floor muscles can also help with achieving orgasm and maintaining control over ejaculation during sexual activity.
But when pelvic floor muscles are weak or tight, they can interfere with sexual function. Men may experience erectile dysfunction or premature ejaculation, while women may have difficulty achieving orgasm or experience pain during intercourse. Also, pelvic floor muscle dysfunction can lead to urinary or fecal incontinence during sex, which can cause sharp pain during sexual intercourse.
Healthy sexual relationships and sexual expression are essential components of overall sexual health. Promoting a positive and respectful approach to sexuality can enhance pleasurable and safe sexual experiences. Talking openly with partners about sexual health, consent, and boundaries is important for building trust and understanding. Everyone should feel empowered to decide what is best for their own sexual health and relationships.
Protecting Against Infections
Safeguarding yourself against sexually transmitted infections (STIs) is a crucial aspect of sexual health. Engaging in safe sexual activity—such as using condoms and dental dams—significantly lowers the risk of STIs and unintended pregnancy. Regular testing and screenings are essential for early detection and effective treatment, helping to maintain healthy sexual relationships and prevent the spread of infections. Being informed about the different types of STIs, their symptoms, and available treatments empowers individuals to make safer choices and seek timely care. By taking proactive steps in prevention and staying up-to-date with testing, you can enjoy sex and build healthy relationships, free from the risks associated with STIs and unintended pregnancy.
Importance of Education and Awareness
Comprehensive education and awareness are the foundation of healthy sexuality and sexual relationships. Access to accurate sexual health information enables individuals to make informed decisions about birth control, STI prevention, and healthy relationships. It’s equally important to address the emotional and psychological aspects of human sexuality, including gender identity, sexual orientation, and the impact of sexual abuse. By fostering a positive and respectful approach to sexuality, individuals can improve their mental health, emotional well-being, and overall quality of life. Healthcare providers play a vital role in offering guidance, support, and education, ensuring that everyone has the resources they need to navigate their sexuality and relationships with confidence and respect.
Pelvic Floor Exercises for Sexual Health Information:
Pelvic floor muscle exercises, also known as Kegels, are a simple and effective way to improve pelvic floor strength and optimize sexual function. These exercises involve contracting and relaxing the pelvic floor muscles, similar to stopping and starting urine flow. To perform Kegels, sit comfortably and squeeze your pelvic floor muscles for a few seconds. Relax for the same amount of time. Repeat this exercise 10-15 times, 3 times per day.
Staying healthy involves more than just exercise—regular health practices like pelvic floor exercises, as well as getting tested for STIs, are important steps in maintaining sexual health and preventing the spread of infections.
Physical Therapy for Pelvic Floor Dysfunction: Benefits for Physical and Mental Health
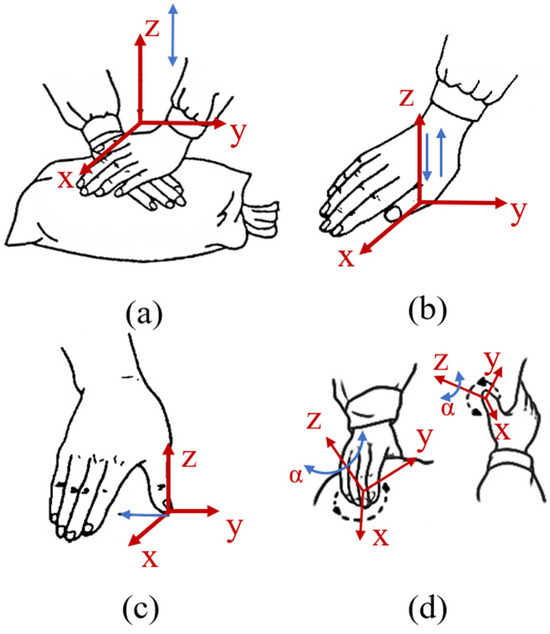
If you are experiencing sexual dysfunction or other symptoms related to pelvic floor muscles, seeking the help of a physical therapist is a wise choice. A physical therapist can evaluate your pelvic floor muscles, develop an individualized treatment plan, and teach you exercises to improve strength and coordination. Treatment may also include manual therapy, biofeedback, and relaxation techniques to help reduce muscle tension and improve sexual function, contributing to better physical and mental health.
Reproductive health is also crucial when addressing pelvic floor dysfunction, as it encompasses access to necessary medical care and services.
In addition to physical therapy, fostering healthy relationships is essential for overall well-being and sexual health.
Health Care and Resources
Access to quality health care and reliable resources is essential for maintaining sexual health and overall well-being. Regular check-ups, screenings, and testing for sexually transmitted infections and other sexual health concerns are vital for early detection and prevention. Healthcare providers should offer comprehensive guidance on birth control options, sexual health education, and support for addressing sexual dysfunction or sexual abuse. Prioritizing sexual health care is especially important for women and adolescents, as it helps prevent cervical cancer, unintended pregnancy, and other health risks. By ensuring that sexual health care is accessible, confidential, and patient-centered, individuals can build healthy, fulfilling sexual relationships and enjoy a higher level of social and emotional well-being.
Conclusion:
Your pelvic floor muscles are an essential component of your overall health, including sexual health. Providing empowering sexual health information can help individuals understand the importance of maintaining strong pelvic floor muscles. By performing pelvic floor exercises and seeking the guidance of a physical therapist, you can improve your pelvic floor function and enhance your sexual experience. Don’t hesitate to seek help if you are experiencing symptoms related to pelvic floor dysfunction. Visit www.pelvis.nyc now!
Remember, a healthy pelvic floor leads to a healthy sex life. It is crucial to adopt a positive and respectful approach to sexual health.