Direct Answer: What Is Proctalgia Fugax During Menstruation?
Proctalgia fugax during menstruation is a sudden, intense spasm of the rectal or pelvic floor muscles that can occur before or during your period. During menstruation, the body releases hormones called prostaglandins that cause the uterus to contract and shed its lining. Prostaglandins can also cause the rectum and pelvic floor muscles around the anal canal to contract, triggering muscle spasms and butthole cramps.
Hormonal changes can affect the bowels and digestive system, leading to symptoms like diarrhea or constipation. These episodes are typically fleeting rectal pain—brief (seconds to minutes) but can feel sharp, cramping, or stabbing. Hormonal fluctuations, uterine contractions, and pelvic floor tension during the menstrual cycle are common triggers. Hormonal changes during menstruation can affect all pelvic floor muscles, not just the uterus, leading to rectal pain.
What Is Proctalgia Fugax?
Proctalgia fugax is a functional anorectal pain condition characterized by sudden, severe rectal pain that comes and goes unpredictably. The exact cause of proctalgia fugax is unknown, but it can be triggered by factors such as stress and constipation. It’s not caused by structural disease, which makes it frustrating—and often misunderstood.
Key Characteristics:
- Sudden, sharp or cramping pain in the rectum (“butthole cramps”)
- Lasts seconds to several minutes
- No visible physical abnormalities
- Often occurs at night or during periods of stress
According to organizations like the American College of Obstetricians and Gynecologists, pelvic pain disorders can be influenced by hormonal and muscular factors, especially during menstruation.
Why Does Proctalgia Fugax Happen During Your Period?

Menstruation triggers a cascade of physiological changes that can directly affect your pelvic floor muscles.
In the days leading up to your period, estrogen and progesterone levels tend to drop dramatically. This sudden hormonal drop can affect the digestive system, often leading to symptoms like diarrhea or constipation, which may trigger anal spasms. Progesterone controls bowel movements, and its decline can create pain by triggering muscle spasms in the pelvic area. Such contractions and hormonal changes can lead to rectal pain by triggering muscle spasms in the pelvic area, contributing to the symptoms of proctalgia fugax during menstruation.
1. Hormonal Fluctuations
During your cycle, prostaglandins (hormone-like chemicals) increase to help the uterus contract and shed its lining. However, these chemicals can also:
- Trigger spasms in nearby muscles
- Increase pain sensitivity
- Affect bowel movements and rectal muscles
2. Pelvic Floor Muscle Tension
Your pelvic floor supports your uterus, bladder, and rectum. During your period:
- Muscles may tighten reflexively due to pain
- Stress and discomfort increase muscle guarding
- This can lead to spasms—felt as sudden rectal pain
3. Uterine Contractions Radiating Pain
The uterus sits close to the rectum. Strong contractions can:
- Refer pain to the anus or rectum
- Feel like deep internal cramps rather than typical menstrual cramps
4. Underlying Pelvic Conditions
Conditions like:
- Endometriosis
- IBS (Irritable Bowel Syndrome)
- Levator ani syndrome
can amplify symptoms during menstruation. Intense period pain, extreme tiredness, and frequent thrush infections can be symptoms of endometriosis. Severe cases of rectal pain during menstruation may indicate underlying conditions such as endometriosis or fibroids.
Symptoms: How to Tell If It’s Proctalgia Fugax or Something Else
Here’s how proctalgia fugax differs from other types of pelvic or rectal pain:
| Symptom | Proctalgia Fugax | Hemorrhoids | Levator Ani Syndrome |
|---|---|---|---|
| Pain duration | Seconds–minutes | Persistent | Longer (20+ minutes) |
| Pain type | Sharp, sudden | Aching, burning | Dull, pressure-like |
| Trigger | Random, menstruation | Straining | Sitting, stress |
| Visible signs | None | Swelling, bleeding | None |
If your pain is brief and intense, especially around your period, it’s likely proctalgia fugax.
If you experience similar symptoms to those listed for other conditions, or if you have severe pain that is sharp, stabbing, or sudden, consult a healthcare provider to rule out other causes.
Why Do I Get Anal Pain or “Butthole Cramps” During My Period?
If you’ve ever felt a sudden, stabbing pain in your rectum during your period—often described as “butthole cramps”—you’re not alone.
This usually happens because:
- The pelvic floor muscles suddenly contract or spasm
- Hormones (like prostaglandins) increase pain sensitivity
- Uterine contractions radiate pain to nearby muscles, including the rectum
This type of pain is commonly linked to proctalgia fugax, a condition involving brief but intense rectal muscle spasms.
Pelvic Floor Dysfunction and Period Pain: What’s the Connection?
Your pelvic floor muscles support your uterus, bladder, and rectum. When these muscles become too tight or uncoordinated, it can lead to:
- Rectal or anal pain
- Deep pelvic pressure
- Pain in the buttocks or hips
- Difficulty relaxing during bowel movements
During menstruation, the body is already under stress from inflammation and contractions. This can cause the pelvic floor to overreact and tighten, leading to pain.
Proctalgia Fugax vs. Levator Ani Syndrome
These two conditions are often confused but have key differences:
| Condition | Pain Type | Duration | Common Trigger |
|---|---|---|---|
| Proctalgia fugax | Sharp, sudden | Seconds–minutes | Hormones, stress |
| Levator ani syndrome | Dull, aching pressure | 20+ minutes | Sitting, chronic tension |
If your pain is quick and intense, it’s more likely proctalgia fugax.
If it’s longer-lasting and persistent, it may be levator ani syndrome.
Other Period Symptoms That May Occur Together
When pelvic floor dysfunction is involved, you may also notice:
- Increased period pain beyond normal cramps
- Painful bowel movements during menstruation
- Lower back or hip tightness
- A feeling of pressure in the rectum
- Fatigue from chronic muscle tension
These symptoms often overlap, which is why they’re frequently misdiagnosed or dismissed.
Can Heavy Bleeding Make Proctalgia Fugax Worse?
Yes, heavy menstrual bleeding can intensify symptoms.
Here’s why:
- Higher prostaglandin levels → stronger muscle contractions
- Increased inflammation → more nerve sensitivity
- Greater physical strain on pelvic muscles
If you experience heavy flow along with anal pain, it’s a strong sign that your pelvic floor may be involved.
Proctalgia Fugax Home Remedies for Period-Related Pain
If your symptoms are occasional, these at-home strategies can help manage discomfort:
Immediate Relief
- Apply a heating pad to the pelvic area
- Take a warm bath to relax muscles
- Practice deep diaphragmatic breathing
Muscle Relaxation
- Focus on pelvic floor relaxation, not tightening (avoid excessive Kegels)
- Try gentle stretching (hips, glutes, lower back)
Lifestyle Support
- Stay hydrated
- Avoid constipation triggers
- Reduce caffeine if it worsens symptoms
These methods can help reduce the intensity of spasms—but they don’t always address the root cause.
If these strategies don’t help, consider working with pelvic floor specialists at Pelvis NYC for personalized care.
The Role of the Pelvic Floor in Period Pain
The pelvic floor is often overlooked in menstrual health. When these muscles become tense or overactive, they can contribute to the pain-tension cycle, making symptoms like proctalgia fugax during menstruation worse. Gentle exercise, such as walking or stretching, can support healthy blood flow to the pelvic area and help prevent intense cramping and muscle spasms.
What Happens During Your Period:
- Increased uterine activity → muscle guarding
- Pain signals → involuntary tightening
- Stress/anxiety → further tension
This creates a pain-tension cycle:
Pain → Muscle tightening → Reduced blood flow → More pain
Breaking this cycle is essential—and this is where physical therapy becomes powerful.
Related Blog: How to Relieve Anal Pain and Improve Pelvic Floor Health through Proctalgia Fugax Exercises?
Why Pelvic Floor Physical Therapy Is a Game-Changer
Pelvic floor physical therapy (PFPT) is one of the most effective treatments for recurrent proctalgia fugax, especially when linked to menstruation. In clinical practice, pelvic floor physical therapy is an evidence-based approach to managing pain in the pelvic area.
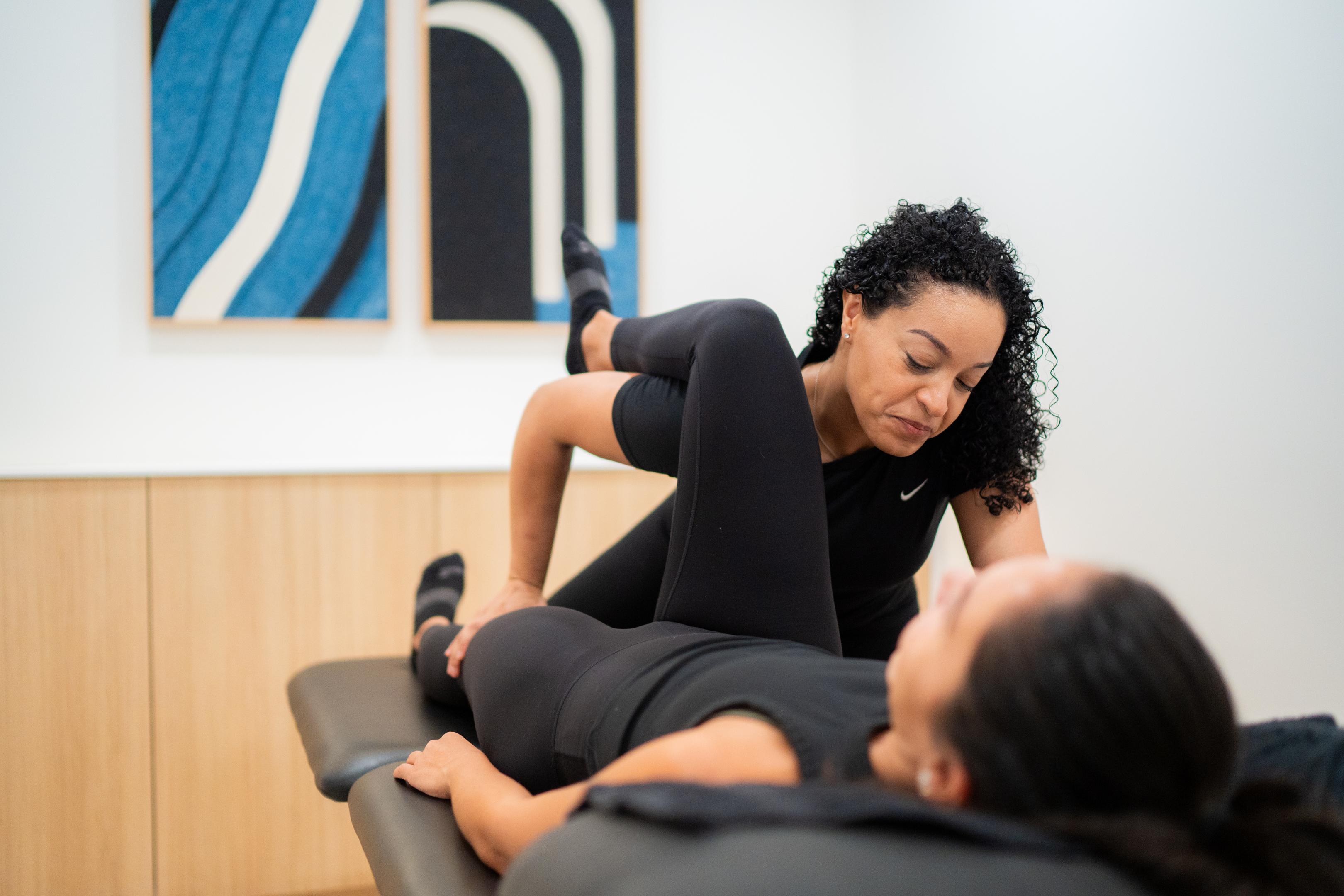
What a Pelvic Floor PT Does:
- Assesses muscle tone, strength, and coordination
- Identifies trigger points in pelvic muscles
- Teaches relaxation techniques
- Uses manual therapy to release tension
Evidence-Based Benefits:
According to research from the National Institutes of Health:
- Pelvic floor therapy significantly reduces chronic pelvic pain
- Improves muscle coordination
- Decreases frequency of spasms
Techniques Used:
- Biofeedback training
- Myofascial release
- Breathing exercises
- Stretching and mobility work
Real-Life Insight: Why Many Women Miss This Diagnosis
Many women are told:
- “It’s just period pain”
- “It’s normal cramps”
But sharp rectal pain during menstruation is real pain—not just a part of having periods. It is not something you have to live with.
Pelvic floor dysfunction is underdiagnosed because:
- Symptoms are internal and invisible
- Many women feel embarrassed discussing anal pain
- General practitioners may not specialize in pelvic health
Proctalgia Fugax Home Remedies (That Actually Help)
If you’re dealing with occasional episodes, these strategies can provide relief:
Staying hydrated and eating more fiber-rich foods can help prevent constipation and ease pain.
9.1 Immediate Relief
- Taking over-the-counter pain relievers can help ease pain and discomfort associated with proctalgia fugax menstruation.
- Warm baths or compresses can help relax the muscles in the anus and rectum, reducing cramping.
- Practicing relaxation techniques, such as deep breathing, can help reduce pain and discomfort during menstruation.
9.2 Ongoing Self-Care
- Light exercise, such as walking or stretching, can support healthy blood flow and help prevent muscle spasms.
- Using healthy toileting techniques, such as elevating the knees while sitting on the toilet, can help relax pelvic floor muscles and ease bowel movements.
Immediate Relief:
- Warm bath or heating pad
- Deep diaphragmatic breathing
- Gentle pelvic floor relaxation (not Kegels!)
Lifestyle Adjustments:
- Reduce caffeine (can trigger spasms)
- Stay hydrated
- Manage constipation
During Your Period:
- Magnesium supplements (may reduce muscle spasms)
- Anti-inflammatory foods
- Gentle stretching (hips, glutes, pelvis)
When to See a Specialist
You should seek professional help if:
- Pain is frequent or worsening
- Episodes disrupt sleep or daily life
- You also experience heavy bleeding or severe cramps
- The pain lasts longer than 20 minutes, or is severe—consult a medical professional
A pelvic floor physical therapist or gynecologist can rule out:
- Endometriosis
- Fibroids
- Chronic pelvic pain disorders
If symptoms are severe or persistent, it is important to consult a medical professional for proper diagnosis and treatment.
Heavy Bleeding and Proctalgia Fugax: Is There a Link?
Heavy menstrual bleeding can intensify pelvic symptoms. The shedding of endometrial tissue during menstruation can contribute to pelvic pain and cramping, as the contractions needed to expel this tissue may also affect the pelvic floor and surrounding muscles. Hormonal fluctuations during the menstrual cycle can also cause symptoms like hormonal acne.
Why?
- More prostaglandins → stronger contractions
- Increased inflammation → heightened pain sensitivity
- Fatigue → reduced muscle recovery
If you have both:
- Severe cramps
- Heavy flow
- Rectal pain
…it’s worth a deeper evaluation.
CTA: Get Expert Help at Pelvis NYC
If you’re experiencing recurring anal pain during your period, working with specialists can change everything.
Pelvis NYC offers expert pelvic floor physical therapy tailored specifically for women dealing with:
- Proctalgia fugax
- Period-related pelvic pain
- Levator ani syndrome
Their evidence-based approach helps you:
- Relax overactive pelvic muscles
- Reduce pain episodes
- Restore normal function
👉 Don’t ignore the pain—address the root cause with professional guidance. Schedule a consultation now!
Frequently Asked Questions (FAQs)
What causes sharp anal pain during my period?
Sharp anal pain during menstruation is usually caused by pelvic floor muscle spasms triggered by hormonal changes and uterine contractions.
Is proctalgia fugax dangerous?
No, it’s not dangerous, but it can be very painful and disruptive. Persistent symptoms should be evaluated.
How long does proctalgia fugax last?
Episodes typically last from a few seconds to several minutes.
Can pelvic floor therapy really help?
Yes, pelvic floor physical therapy is one of the most effective treatments for reducing muscle spasms and preventing recurrence.
Is this related to endometriosis?
It can be. Endometriosis may cause referred rectal pain, especially during menstruation.
Why does it feel like “butthole cramps”?
This sensation comes from sudden contractions of the pelvic floor muscles surrounding the rectum.
Final Thoughts
Proctalgia fugax during menstruation is more common than most women realize—and far more treatable than you’ve probably been told. Understanding the role of your pelvic floor is the key to breaking the cycle of pain.
You don’t have to normalize discomfort that disrupts your life. With the right support, especially through pelvic floor physical therapy, relief is absolutely possible.



