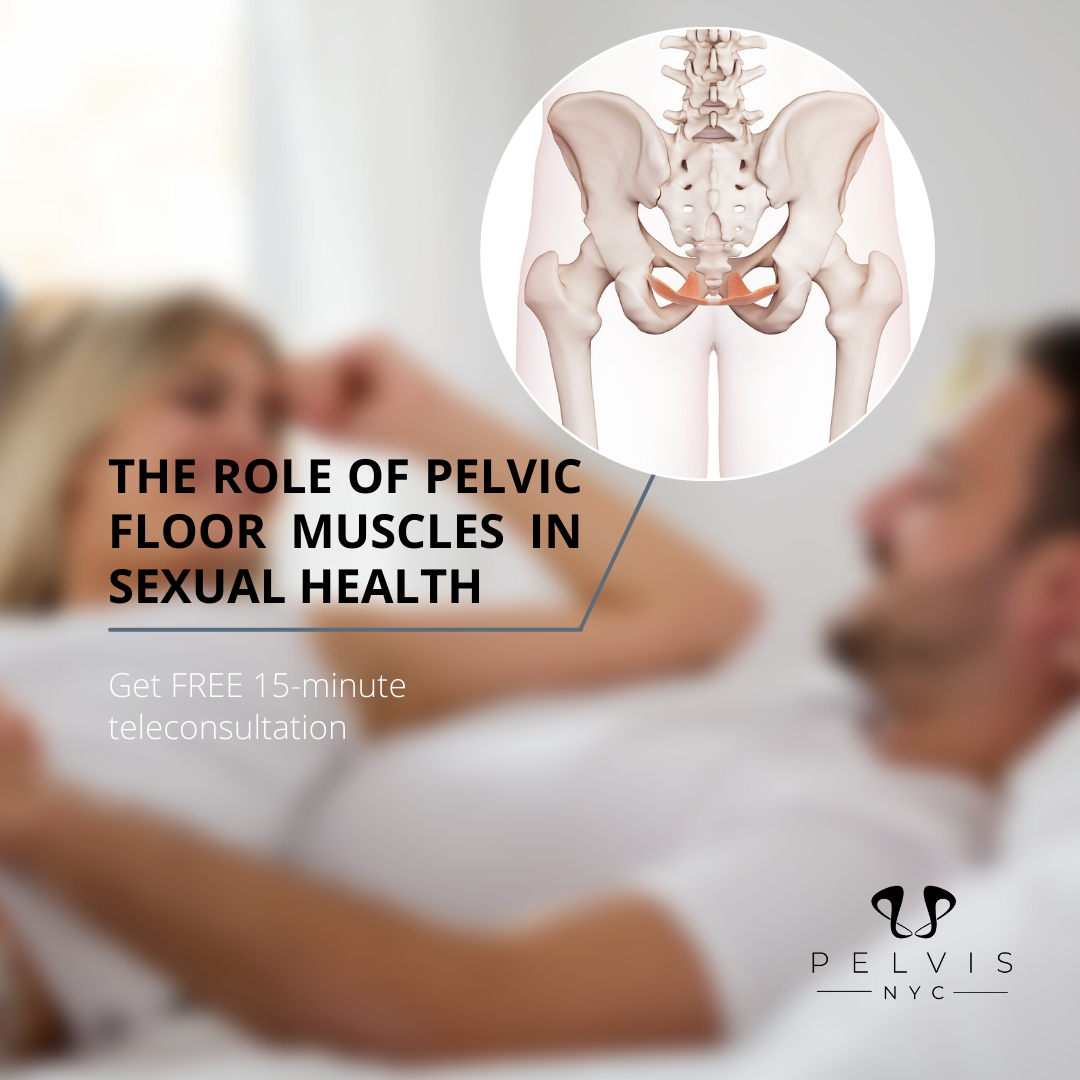
Pelvic Floor Health for Men: Why It Matters
Pelvic floor health is essential for men because the pelvic floor muscles support bladder control, bowel function, sexual performance, and core stability. When these muscles become weak, tight, or uncoordinated, men may experience symptoms like urinary leakage, erectile dysfunction, pelvic pain, or discomfort after prostate surgery.
The good news: many pelvic floor disorders can improve significantly with targeted pelvic floor exercises and pelvic floor physical therapy. Early treatment often prevents symptoms from becoming chronic and improves quality of life.
What Is Pelvic Floor Health?

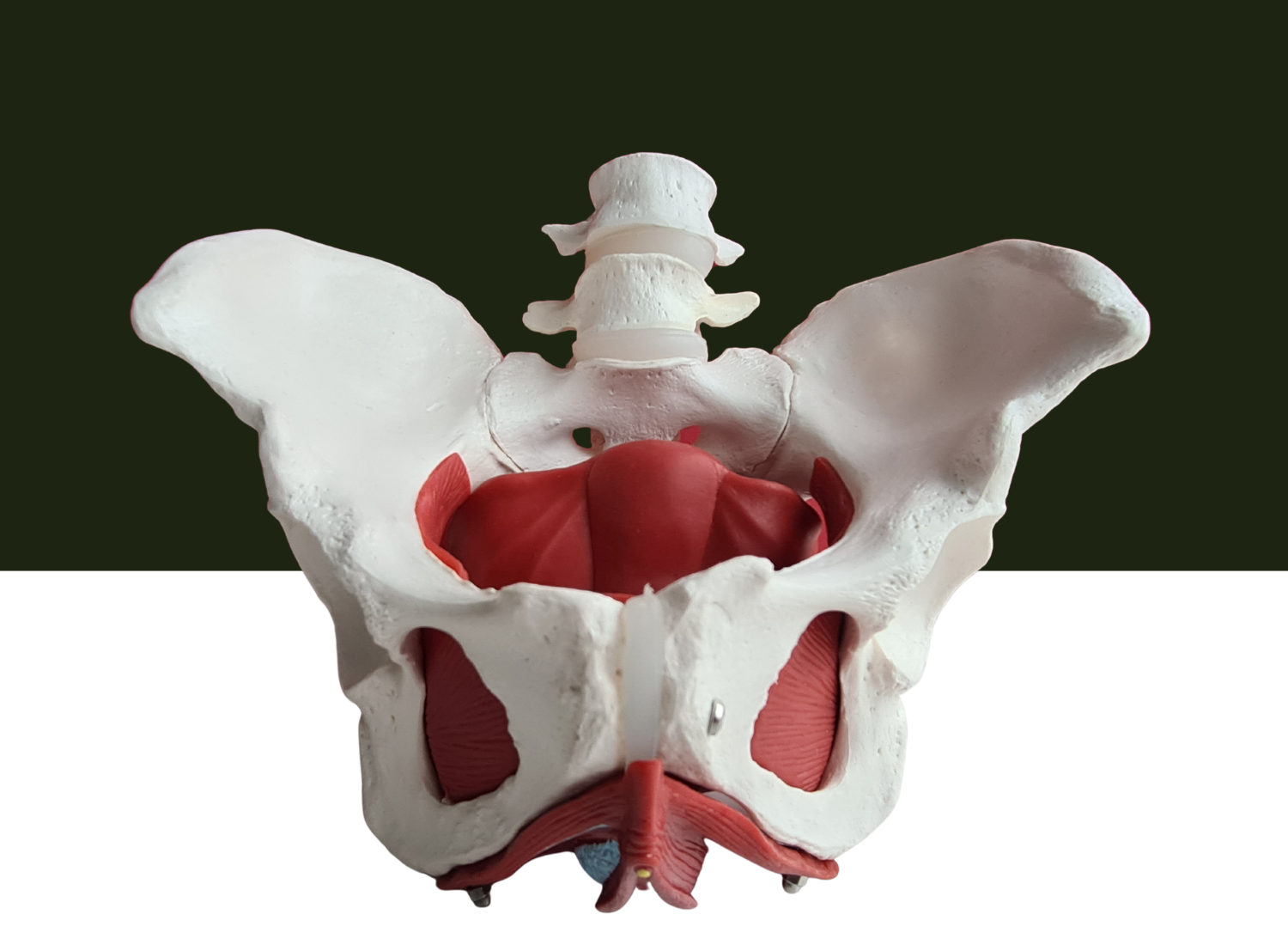
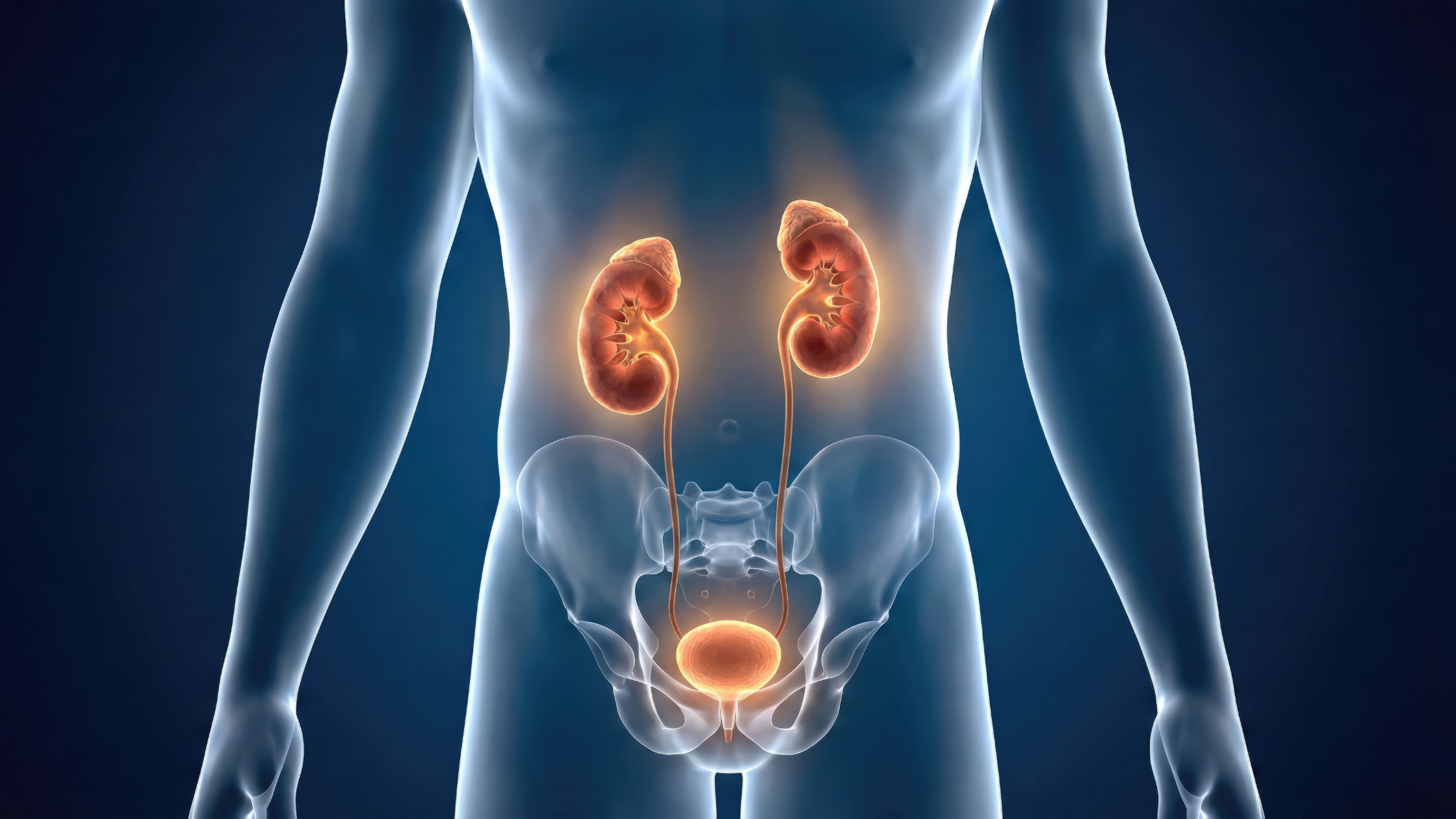
Pelvic floor health refers to the proper function of the muscles, connective tissues, and nerves located at the bottom of the pelvis. These muscles form a sling-like structure that supports internal organs, including the bladder, bowel, and prostate.
For men, a healthy pelvic floor helps with:
- Bladder and bowel control
- Sexual function and erectile strength
- Core stability and posture
- Pressure management during lifting or exercise
- Recovery after prostate procedures
Many men don’t realize these muscles exist until symptoms appear. However, pelvic floor dysfunction is more common than most people think.
According to the National Institutes of Health (NIH), millions of men experience pelvic floor disorders, particularly after prostate surgery, chronic straining, aging, or high-impact physical activity.
Understanding the Pelvic Floor Muscles
What Are Pelvic Floor Muscles?

The pelvic floor muscles stretch from the pubic bone in the front to the tailbone in the back. They support the pelvic organs and help control urination, bowel movements, and sexual response.
Think of these muscles as part of your body’s “core canister,” working alongside the diaphragm, abdominal muscles, and lower back muscles.
When functioning properly, these muscles:
- Contract to maintain continence
- Relax to allow urination and bowel movements
- Support sexual performance
- Stabilize the pelvis and spine
When they become weak or overly tight, symptoms can develop.
Common Pelvic Floor Dysfunction in Men
What Is Pelvic Floor Dysfunction?
Pelvic floor dysfunction occurs when the muscles or tissues in the pelvic area become weakened or injured and cannot properly contract, relax, or coordinate movement. These pelvic floor conditions affect about 1 in 4 women at some point, and men can also develop these problems. Some men experience weakness, while others experience excessive muscle tension.
Common Symptoms of Pelvic Floor Dysfunction
Men may experience these pelvic floor problems, which can affect quality of life:
- leaking urine or urgency, and sometimes stool leakage, especially with pelvic floor weakness during coughing or laughing
- Difficulty emptying the bladder
- Constipation or straining
- Erectile dysfunction or sexual dysfunction
- Pain in the pelvis, groin, or tailbone
- Pain during or after ejaculation
- Lower back, hip, or tailbone discomfort linked to core dysfunction in the pelvic floor
- Pressure or heaviness in the pelvic region
Symptoms may develop gradually and are often mistaken for “normal aging.”
Pelvic Floor Disorders Men Should Know About
1. Urinary Incontinence
Urinary leakage is one of the most common pelvic floor disorders in men, especially after prostate surgery.
A 2023 review published in European Urology found that pelvic floor muscle training significantly improved continence recovery after prostatectomy.
Common Signs:
- Leaking during coughing or exercise
- Frequent urination
- Sudden urges to urinate
- Nighttime bathroom trips
2. Erectile Dysfunction
Weak or poorly coordinated pelvic floor muscles can reduce blood flow control and affect erectile quality.
Research published in The Journal of Sexual Medicine showed that men who performed pelvic floor exercises consistently experienced improvements in erectile function compared to those receiving lifestyle advice alone.
3. Chronic Pelvic Pain Syndrome(CPPS)
CPPS affects approximately 2–16% of men globally and often involves muscle tension, nerve irritation, and stress-related muscular guarding; in some patients, it can overlap with other pelvic health conditions such as interstitial cystitis or irritable bowel syndrome.
Symptoms include:
- Pelvic aching
- Testicular pain
- Burning sensations
- Pain with sitting
- Pain after urination or ejaculation
Many men benefit from pelvic floor physical therapy focused on relaxation and coordination—not just strengthening.
4. Pelvic Organ Prolapse in Men
Although less common than in women, pelvic organ prolapse can occur in men, particularly after surgery or chronic straining.
This happens when pelvic structures lose support due to muscle weakness or connective tissue dysfunction.
Risk factors include:
- Chronic constipation
- Heavy lifting
- Obesity
- Persistent coughing
- Pelvic surgery history
Why Pelvic Floor Health Is Important for Men
Better Bladder Control
A strong pelvic floor helps support both bladder and bowel control, reducing leakage and urgency.
This is particularly important for:
- Athletes
- Aging men
- Men recovering from prostate procedures
Improved Sexual Health
The pelvic floor muscles contribute directly to erectile rigidity, ejaculatory control, and sexual arousal.
Improving muscle coordination may help:
- Enhance erections
- Improve stamina
- Increase pelvic blood flow
- Reduce discomfort during intimacy
Reduced Pelvic Pain
Tight pelvic muscles can compress nerves, and therapy may help release tension and relieve pain.
Pelvic floor therapy often helps men:
- Reduce pain flare-ups
- Improve mobility
- Return to exercise comfortably
- Sit without discomfort
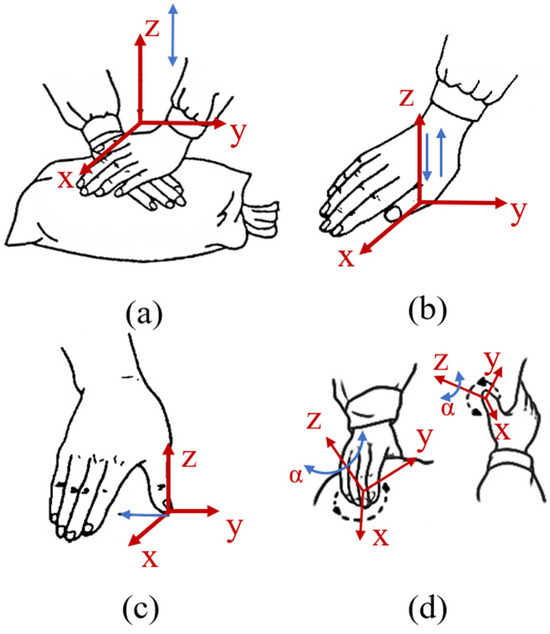
Hands-on techniques such as myofascial release may also be used, especially when scar tissue or other restricted tissues contribute to symptoms.
Better Core Stability and Athletic Performance
The pelvic floor works closely with the core and breathing system. High-impact exercises such as running, jumping, or heavy lifting create significant downward pressure on the pelvic organs.
Poor pelvic floor function can affect:
- Squat mechanics
- Deadlifting stability
- Running performance
- Pressure management during sports
Many athletes unknowingly overload the pelvic floor by holding their breath or bracing improperly during heavy lifting, and improving pelvic floor strength depends on more than strengthening alone and also requires coordination and behavioral changes.
Pelvic Floor Exercises for Men
Do Kegel Exercises Actually Work?
Yes—when performed correctly.
Kegel exercises involve a pelvic floor contraction—tightening the pelvic floor muscles as if trying to hold in urine, holding for several seconds, and then releasing—to improve strength, endurance, and coordination.
However, many men perform them incorrectly or over-tighten already tense muscles.
How to Identify the Right Muscles
Imagine stopping urine flow midstream or preventing passing gas. Those are your pelvic floor muscles.
Basic Kegel Exercise
- Tighten the pelvic floor muscles gently
- Hold for 3–5 seconds
- Relax fully for 5 seconds
- Repeat 10 times
Aim for:
- 2–3 sessions daily
- Consistent breathing
- No excessive abdominal tightening
When Kegels Can Make Symptoms Worse
Not every pelvic floor issue requires strengthening.
If muscles are overly tight, Kegel exercises may increase:
- Pelvic pain
- Urinary urgency
- Muscle tension
- Sexual discomfort
This is why assessment by a pelvic floor physical therapist matters.
The Role of Pelvic Floor Physical Therapy
What Is Pelvic Floor Physical Therapy?
Pelvic floor physical therapy is a specialized treatment approach that evaluates and treats pelvic muscle dysfunction.
A trained physical therapist assesses:
- Muscle strength
- Coordination
- Breathing mechanics
- Posture
- Core function
- movement patterns
Pelvic therapy begins with an initial evaluation, including a detailed medical history and a physical exam of pelvic floor muscle function, before creating a personalized plan based on symptoms and goals.
What Happens During Pelvic Floor Therapy Sessions?

Many men feel nervous before their first appointment, but therapy sessions are educational, professional, and tailored to comfort levels. Depending on your symptoms, physical therapy sessions may also use different treatment techniques and specialty equipment to see what works best.
- Health history and goals
- Symptom review, including bladder and bowel function
- External and internal muscle assessment (if appropriate and with consent)
- Posture, breathing, and movement patterns
- Hands-on treatment to release tight tissues or improve coordination
- A customized exercise plan
- Biofeedback therapy to assess muscle activity, improve control, and track progress
- Electrical stimulation when indicated to help reduce pain and support muscle function
- Education on proper body mechanics and self-care strategies
Treatment is personalized and may also include lifestyle modifications, along with exercises, manual therapy, and education.
A Typical Pelvic Floor Therapy Appointment May Include:
- Symptom review
- Movement assessment
- Breathing analysis
- Postural evaluation
- Core stability testing
- Guided pelvic floor exercises
- Relaxation techniques
- Manual therapy if appropriate
Treatment often focuses on both strengthening and relaxation.
Why Physical Therapy Matters
Physical therapy can address the root cause of many pelvic floor issues—not just symptoms.
A pelvic floor physical therapist can help:
- Improve bladder control
- Relieve pain through individualized care from a pelvic floor therapist
- Restore sexual function
- Improve exercise mechanics
- Prevent unnecessary surgery
- Speed recovery after prostate surgery
A 2022 meta-analysis published in Physical Therapy Journal found pelvic floor rehabilitation significantly improved urinary symptoms and quality of life in men after prostate treatment.
Lifestyle Habits That Support Pelvic Floor Health
1. Avoid Chronic Straining
Straining during bowel movements places excessive pressure on the pelvic floor and can contribute to bowel dysfunction.
Support bowel health with:
- High-fiber foods
- Hydration
- Proper toilet posture
2. Manage Heavy Lifting Correctly
Poor lifting mechanics increase abdominal pressure and strain pelvic tissues.
Tips:
- Exhale during exertion
- Avoid breath-holding
- Use proper form
- Strengthen the core gradually
3. Maintain a Healthy Weight
Excess body weight increases pelvic pressure and may worsen symptoms.
Even modest weight loss can improve:
- Urinary control
- Pelvic pain
- Exercise tolerance
4. Reduce High Stress Levels
Stress often contributes to chronic pelvic muscle tension.
Helpful strategies include:
- Deep breathing
- Walking
- Stretching
- Mindfulness exercises
- Guided relaxation
When Should Men See a Pelvic Floor Specialist?
Signs You Should Book a Pelvic Floor Therapy Appointment
Seek professional evaluation if you experience:
- Persistent pelvic pain
- Urinary leakage
- Erectile dysfunction
- Pain after prostate surgery
- Pain during sitting
- Constipation or straining
- Pressure in the pelvis
- Ongoing hip or groin tension
Early treatment typically leads to better outcomes.
How Pelvis NYC Helps Men Improve Pelvic Floor Health

If you’re dealing with pelvic floor dysfunction, you do not have to manage it alone.
Pelvis NYC specializes in evidence-based pelvic floor physical therapy for men. Their team helps patients improve bladder control, reduce pelvic pain, restore sexual health, and recover after surgery through personalized treatment plans, while supporting men through personalized pelvic health and women’s health-informed care.
Whether you’re experiencing urinary issues, pelvic discomfort, or core instability, scheduling a pelvic floor therapy appointment can be the first step toward lasting relief.
Pelvis NYC also offers consultations to help men better understand their symptoms and treatment options.
Frequently Asked Questions About Pelvic Floor Health
What are the symptoms of pelvic floor dysfunction in men?
Symptoms may include urinary leakage, pelvic pain, erectile dysfunction, constipation, urgency, and discomfort while sitting.
Can pelvic floor exercises help erectile dysfunction?
Yes. Research suggests pelvic floor exercises may improve erectile function by strengthening muscles involved in blood flow control and sexual performance.
Are Kegel exercises safe for all men?
Not always. Some men have overly tight pelvic floor muscles, and excessive Kegels may worsen symptoms. A pelvic floor physical therapist can determine the right approach.
How long does pelvic floor physical therapy take?
Most men notice improvements within several weeks, though timelines vary depending on symptom severity and treatment adherence.
Is pelvic floor dysfunction common after prostate surgery?
Yes. Urinary leakage and pelvic weakness are common after prostatectomy, but pelvic floor physical therapy can significantly improve recovery outcomes.
What happens during pelvic floor therapy sessions?
Sessions may include movement assessments, breathing exercises, muscle coordination training, posture correction, manual therapy, and guided exercises. Therapists may also assess muscle tone and use techniques such as biofeedback therapy or electrical stimulation when appropriate.
Final Thoughts
Pelvic floor health is a foundational part of men’s physical wellness, affecting bladder control, sexual performance, mobility, and overall quality of life. Yet many men delay treatment because they don’t realize effective help exists.
The earlier pelvic floor dysfunction is addressed, the easier it is to improve symptoms and prevent long-term complications. Whether you’re recovering from surgery, dealing with pelvic pain, or simply looking to improve core function and confidence, pelvic floor physical therapy can make a measurable difference.
If symptoms are affecting your daily life, consider scheduling a consultation with Pelvis NYC to begin a personalized recovery plan.